The Seed Oil Scandal: Why Common Cooking Oils Are Under Fire, What the Science Really Says, and What Actually Is Making the Western World Sick
You’ve probably seen the headlines. “Seed oils are poison.” “These 4 oils are destroying your health.” Maybe someone in your social feed has declared canola oil the nutritional equivalent of motor fuel. And you’ve started quietly wondering whether the stir-fry you had for dinner last night is slowly killing you.
Here’s the thing: the story is more complicated than the viral posts suggest. And buried beneath all the noise is a genuinely important conversation about how modern food, especially restaurant food, is affecting your health. Just maybe not in the way you’ve been told.
Introduction
The Western world is undeniably dealing with a chronic disease crisis. Obesity, type 2 diabetes, cardiovascular disease, and metabolic syndrome are rising in tandem across North America, Europe, Australia, and beyond. Understandably, people want answers. They want a villain.
Enter seed oils.
Over the past several years, a wave of wellness influencers, podcasters, and internet personalities have pointed the finger squarely at cooking oils like canola, corn, soybean, and sunflower, claiming they are the root cause of inflammation, obesity, cancer, and practically every ailment of modern civilization. The theory sounds compelling. Consumption of these oils has increased dramatically over the past century. So has chronic disease. The logic feels intuitive, almost inevitable.
But intuition and evidence are not the same thing. And when you look closely at the peer-reviewed science, a different picture emerges. Seed oils, it turns out, are not the dietary villains they’ve been painted as. What IS genuinely making people sick is more nuanced, less clickable, and arguably more important to understand.
This article lays it all out. We’ll examine what seed oils actually are, what the science really says about them, and what the legitimate culprits are in our modern food environment, including the restaurant meals most of us eat several times a week without thinking twice.
Medical Disclaimer: The information in this article is intended for general educational purposes only. It does not constitute medical advice, diagnosis, or treatment. Before making any significant changes to your diet or lifestyle, please consult a qualified healthcare professional, such as a registered dietitian or your primary care physician.
Section 1: What Are Seed Oils, and Why Are They Suddenly Controversial?
Seed oils are exactly what the name suggests: oils pressed or extracted from the seeds of plants. Canola (from rapeseed), corn, soybean, sunflower, safflower, grapeseed, cottonseed, and rice bran oil all fall into this category. They became staples of the modern food supply throughout the 20th century, initially promoted as heart-healthier alternatives to animal fats like lard and butter.
For decades, major health organizations including the American Heart Association supported their use, largely because they are high in polyunsaturated fatty acids (PUFAs), particularly omega-6 fatty acids. Replacing saturated fats with these oils was associated with lower LDL (“bad”) cholesterol and reduced cardiovascular risk in large studies.
Then social media arrived.
Starting around 2018 and accelerating rapidly through the pandemic years, the anti-seed oil movement exploded online. Critics labeled canola, corn, cottonseed, soybean, sunflower, safflower, grapeseed, and rice bran oil as the “hateful eight,” claiming these oils cause inflammation, weaken immunity, drive obesity, and trigger chronic disease. The theories spread fast because they tapped into something real: the sense that something in our modern food supply is genuinely wrong. And that instinct, even if misdirected at seed oils specifically, is not entirely wrong.
Section 2: The Seed Oil Inflammation Theory, What the Science on Cooking Oils Actually Says
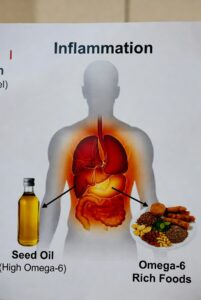
The central claim against seed oils is this: they are high in omega-6 fatty acids, which supposedly promote inflammation in the body, and since inflammation underlies most chronic disease, seed oils must be driving the epidemic.
This argument has a fatal flaw: the evidence doesn’t support it.
Christopher Gardner, PhD, director of nutrition studies at the Stanford Prevention Research Center and former chair of the American Heart Association’s Nutrition Committee, has studied dietary fats for more than three decades. His assessment is blunt. “There is abundant evidence suggesting that seed oils are not bad for you. If anything, they are good for you,” he told Johns Hopkins’ Bloomberg School of Public Health. The confusion, he explains, stems from a misreading of how omega-3 and omega-6 fatty acids actually work.
Omega-3 fats have somewhat stronger anti-inflammatory properties than omega-6 fats. Somewhere along the way, this nuance got translated into the claim that omega-6 fats are pro-inflammatory, which is simply not what the science shows. According to nutrition researchers at Johns Hopkins Bloomberg School of Public Health, seed oils do not cause inflammation, and research actually links linoleic acid (the main omega-6 in seed oils) to a 35% lower risk of developing type 2 diabetes.
The American Heart Association, Memorial Sloan Kettering Cancer Center, and the World Cancer Research Fund have all stated clearly that consuming seed oils at normal dietary amounts is not linked to increased inflammation, cancer, or cardiovascular disease. A 2025 study in the journal Nutrients, covering nearly 3,000 people, found no connection between linoleic acid levels in the blood and markers for inflammation.
So what is the problem? Where does the confusion come from?
Here’s the short answer: it comes from what seed oils are in.
Section 3: The Real Culprit: Ultra-Processed Foods Loaded with Cooking Oils, Salt, and Sugar
Seed oils don’t exist in a vacuum. They are a key ingredient in virtually every ultra-processed food on the market. Packaged snacks, fast food, frozen meals, commercial baked goods, and most chain restaurant dishes contain seed oils in combination with enormous amounts of added sugar, refined carbohydrates, sodium, additives, emulsifiers, preservatives, and very little fiber or nutritional value.
This is the actual problem. Not the oil itself, but the industrial food system it’s part of.
Matti Marklund, PhD, an assistant professor in International Health at Johns Hopkins, sums it up clearly: “We know that ultra-processed foods generally are not good for your health. They are usually high in sodium or salt, added sugars, unhealthy fats, and additives. That’s why it’s bad for you, not the inclusion of seed oils.”
The evidence against ultra-processed foods (UPFs) is, frankly, staggering. A landmark 2024 review published in the British Medical Journal, covering 45 meta-analyses and nearly 10 million study participants, found that higher consumption of ultra-processed foods is associated with 32 different health conditions. These include heart disease, stroke, type 2 diabetes, obesity, depression, anxiety, several cancers, and increased mortality from all causes. A smaller but powerful NIH clinical trial found that people on a high-UPF diet spontaneously consumed 500 more calories per day than those eating minimally processed foods, even when meals were matched for calorie content, fat, protein, sugar, sodium, and fiber.
The foods don’t just contain bad ingredients. They’re engineered to make you eat more than you intend to, regardless of what oil they’re cooked in.
Section 4: Hidden Sodium in Restaurant Food, The Silent Blood Pressure Bomb
Let’s talk restaurants, because this is where the real nutritional story gets uncomfortable.
The FDA recommends no more than 2,300 milligrams (mg) of sodium per day. That’s roughly one teaspoon of table salt. Most Americans are consuming significantly more than that, and restaurant food is a major reason why.
A government-sponsored analysis found that sodium levels in over half of the 125 popular restaurant and fast-food items studied exceeded the FDA’s own sodium limits for using the word “healthy” on packaging. The average American adult is consuming somewhere in the region of 3,400 to 3,700 mg of sodium daily, with restaurant meals accounting for a disproportionate share.
Consider some real numbers from popular chain restaurants:
- A single burrito at a major chain: up to 4,100 mg sodium (nearly two days’ worth)
- Fish and chips at a casual dining restaurant: up to 4,500 mg sodium
- A large Italian sandwich at a chain sub shop: over 4,000 mg sodium
- A pasta dish at a sit-down Italian chain: enough sodium to cover three full days
And that’s before you add a side dish, a soda, or a dressing.
Excess sodium doesn’t just raise blood pressure (though it does that very effectively). It stresses the kidneys, increases the risk of stroke, contributes to fluid retention, and over time raises cardiovascular risk in ways that compound quietly for years before becoming clinically obvious. It’s not dramatic. It doesn’t feel like anything at the time. But it adds up, meal by meal.
Section 5: Added Sugars Are Lurking Where You’d Least Expect Them
You know dessert has sugar. What you probably don’t know is that the grilled salmon, the “healthy” salad, the pasta sauce, and the teriyaki bowl do too.
Added sugar in restaurant food is one of the most underappreciated dietary hazards for frequent diners. Chefs and food scientists know exactly what sugar does to flavor profiles: it rounds out harsh notes, extends palatability, and keeps people coming back. So they add it almost everywhere, often in amounts that would shock you if you could see them measured out.
Common restaurant sugar traps include:
- Salad dressings: A single serving of many commercial or restaurant dressings contains 5 to 10 grams of added sugar. Order a full entrée salad and you might be looking at two or three servings of dressing.
- Barbecue and teriyaki sauces: Often contain 10 to 20 grams of sugar per serving, sometimes more.
- Pasta sauces: Many marinara and vodka sauces at restaurant chains use added sugar to balance acidity.
- Coleslaw and salads with fruit: These are often dressed with sweet vinaigrettes or honey-based dressings.
- “Healthy” smoothies and juices: A large fruit smoothie at a chain outlet can contain 60 to 80 grams of sugar, more than in a can of cola.
- Bread and rolls served before meals: Many restaurant bread products include sugar and refined flours that spike blood glucose before your entrée even arrives.
The American Heart Association recommends women limit added sugar to 25 grams per day and men to 36 grams. A single restaurant meal, if you’re not looking carefully, can blow past those limits before the entrée is even served.
Section 6: Portion Distortion, How Restaurant Serving Sizes Warp Your Perception of Normal
Perhaps the most insidious feature of modern restaurant dining isn’t what’s in the food. It’s how much of it you’re given.
Research from the Journal of the Academy of Nutrition and Dietetics found that over a 30-year period, fast-food portion sizes increased significantly, with dessert portions growing by 24 grams per decade and calories in entrées climbing by 30 calories per decade. This might not sound dramatic, but compounded across thousands of meals over a lifetime, it reshapes what “normal” looks like.
Studies from NYC chain restaurants found that 23% of full-service restaurant patrons consumed at least 2,000 calories in a single visit. That’s a full day’s worth of calories in one meal. Another 76% exceeded the 750-calorie benchmark suggested by health researchers as a reasonable single-meal target.
When you eat at a restaurant regularly, your internal “portion calibration” drifts. The enormous plate becomes the reference point. You start serving yourself larger portions at home. You feel unsatisfied with smaller, more appropriate servings. The effect is gradual, but it’s real, and it’s backed by solid behavioral nutrition research.
Restaurant portions are not designed around your body’s actual energy needs. They’re designed around perceived value, visual appeal, and the expectation that “more” signals generosity. Eating half and boxing the rest is genuinely one of the most impactful habits frequent diners can develop.
Section 7: The Dishes That Look Healthy But Really Aren’t
This section might sting a little, but it’s important.
Some of the most nutritionally problematic items at restaurants are the ones marketed as lighter, fresher, or healthier. The word “healthy” on a menu is often doing more marketing work than nutritional work. Here are some of the most common offenders:
The “Grilled Chicken Salad” Grilled chicken on greens sounds like a win. But add crispy noodles, candied walnuts, dried cranberries, shredded cheese, and a generous ladle of honey-sesame dressing, and you’ve got a meal with 800 to 1,000 calories, 40+ grams of fat, and 30+ grams of sugar. The chicken didn’t do that. The everything-else did.
The Veggie Wrap A whole-wheat tortilla stuffed with roasted vegetables sounds virtuous. But large flour tortillas can contain 300 calories and 600 mg of sodium before anything is added to them. Add hummus, cheese, avocado spread, and a creamy sauce, and you’re looking at a 900-calorie item with sodium levels rivaling a fast-food burger.
The Sushi Platter Plain sashimi is excellent. But most restaurant sushi includes white rice (prepared with rice vinegar and sugar), mayonnaise-based sauces, tempura ingredients, and sweet soy glaze. A “healthy” sushi dinner can easily deliver 1,200 calories and 1,800 mg of sodium.
The Stir-Fry Vegetables and lean protein in a wok sounds ideal. The problem is the sauce, which typically contains soy (very high sodium), sugar, cornstarch, and sometimes oyster sauce (also high sodium). A typical restaurant stir-fry can deliver 1,800 to 2,500 mg of sodium in a single dish.
The Smoothie Bowl Trending heavily as a breakfast option. A base of blended frozen fruit, topped with granola, honey, additional fruit, nut butter, and coconut flakes can easily reach 700 to 900 calories and 50+ grams of sugar before you’ve left the café.
None of these meals are terrible once in a while. The issue arises when people eat them three to five times a week thinking they’re making smart choices, because the hidden nutritional load is genuinely significant.
Section 8: What About Canola, Soybean, Sunflower, and Corn Oil Specifically?
Since the article’s premise involves four common cooking oils, let’s look at each one directly and honestly.
Canola Oil Derived from the rapeseed plant and one of the most researched cooking oils in the world. It has one of the lowest ratios of omega-6 to omega-3 fatty acids among common oils, very low saturated fat, and a high smoke point. Multiple large-scale studies associate canola oil consumption with improved lipid profiles and lower cardiovascular risk. The FDA permits the qualified health claim that canola oil may reduce the risk of coronary heart disease.
Soybean Oil The most widely consumed oil in the United States, used extensively in restaurant kitchens and processed foods. It’s high in polyunsaturated fats and contains some omega-3s. Concerns have been raised about its high omega-6 content and its prevalence in ultra-processed foods. However, the oil itself, at normal dietary levels, has not been shown in clinical trials to increase inflammation or cause harm. The concerns are mostly valid when examining the ultra-processed food context, not the oil in isolation.
Sunflower Oil High in vitamin E and linoleic acid. At high temperatures (like deep frying), high-linoleic sunflower oil can degrade and form oxidation products. High-oleic versions are more stable and better suited to high-heat cooking. The issue isn’t sunflower oil per se but using the wrong variety for high-heat cooking repeatedly.
Corn Oil High in polyunsaturated fats, low in saturated fat. Research generally places it in the “neutral to beneficial” category for cardiovascular health when it replaces saturated fats. Like soybean and sunflower oil, corn oil is frequently found in ultra-processed foods, which is where the legitimate health concern lies.
There is one nuanced but legitimate point to acknowledge: the way oils are used matters. High-linoleic oils like standard sunflower oil, when used repeatedly for deep frying at very high temperatures, can oxidize and form compounds (called oxidized linoleic acid metabolites, or OXLAMs) that some researchers believe may contribute to arterial inflammation. This is a real phenomenon, and it’s one reason why the cooking method and oil stability matters, not just the oil type. High-oleic versions of sunflower and safflower oil, which have been modified to be more heat-stable, are significantly better choices for deep frying than their high-linoleic counterparts.
But here’s the important context: most home cooks aren’t deep-frying repeatedly in the same batch of oil. The concern is more relevant to commercial fryers at fast-food restaurants, where oil is used for extended periods at high temperatures. This is another legitimate reason to reduce fast-food consumption, though notably, it’s an argument about how the oil is used in industrial cooking, not about seed oils themselves being inherently toxic.
The pattern you’ll notice: the oil itself, consumed in reasonable amounts as part of a varied whole-foods diet, is not the public health crisis. The crisis is the industrial food system that packages these oils alongside enormous quantities of sugar, sodium, additives, and refined carbohydrates, and the restaurant industry that deploys all of the above in portions far exceeding actual nutritional needs.
Section 9: What to Use Instead, and What Else Actually Matters
If seed oils aren’t the enemy, should you still consider diversifying the fats in your kitchen? Yes, absolutely. Not because canola oil is dangerous, but because variety and context matter in any healthy diet.
Better choices for everyday cooking:
- Extra virgin olive oil: The most evidence-backed oil for health, particularly cardiovascular health. Rich in monounsaturated fats and anti-inflammatory polyphenols. Suitable for low to medium-heat cooking and as a dressing.
- Avocado oil: High smoke point, high in monounsaturated fats, mild flavor. Excellent for high-heat cooking, searing, and roasting.
- Coconut oil: High in saturated fat, so use sparingly. Not as harmful as trans fats, but not as beneficial as olive or avocado oil. Useful in specific cooking contexts for flavor.
- Butter and ghee (in moderation): Better than trans fats, but still high in saturated fat. Fine occasionally, not as a primary cooking fat.
- Canola or high-oleic sunflower oil: Perfectly reasonable everyday options, particularly for high-heat cooking where olive oil would smoke.
Beyond oil choices, the truly impactful dietary shifts are:
- Reducing ultra-processed food consumption across the board
- Cooking more meals at home where you control ingredients
- Prioritizing whole foods: vegetables, legumes, whole grains, lean proteins, and fruit
- Being aware of sodium, sugar, and portion size when dining out
- Reading nutrition labels with a focus on added sugar and sodium, not just calories
These changes have vastly more impact on long-term health than swapping one oil for another.
Step-by-Step Guide: How to Identify and Order Healthier Meals at Restaurants
You don’t have to stop eating out. You just have to get smarter about it. Here’s a practical, pressure-free approach.
Step 1: Look up the menu before you go. Most chain restaurants publish full nutrition information online. Spend two minutes before you leave home. You’ll make a much more rational decision before you’re hungry, surrounded by appetizing smells, and sitting next to the bread basket.
Step 2: Choose your protein wisely. Grilled, baked, poached, or steamed proteins are almost always better than fried, crispy, or glazed. Ask about preparation methods if the menu doesn’t specify.
Step 3: Request sauces and dressings on the side. This one simple habit can cut your sodium and sugar intake dramatically without sacrificing flavor. Dip your fork in the dressing rather than pouring it over. You’ll use about a quarter of the amount.
Step 4: Watch the “healthy-sounding” descriptors. “Fresh,” “light,” “garden,” and “harvest” on a menu are marketing words, not nutritional guarantees. Look at what’s actually in the dish, not just what the name suggests.
Step 5: Treat the bread basket as optional. Restaurant bread is typically white flour with butter, and it’s placed in front of you before you’ve had a chance to calibrate your hunger. Ask for it to be removed, or commit to one piece only.
Step 6: Reframe the portion. If the restaurant is known for large portions, mentally decide before the food arrives that you’re eating half and taking the rest home. This is easier to stick to if you decide before you start eating rather than when you’re already full and staring at a half-finished plate.
Step 7: Swap the default sides. Most restaurants will substitute a side salad, steamed vegetables, or a fresh fruit cup for fries if you ask. Sometimes there’s a small upcharge. It’s usually worth it.
Step 8: Be specific about modifications. Asking for a dish “without the sauce” or “with olive oil instead of the house dressing” is completely normal in most restaurants. Staff are used to it. Be polite, be specific, and don’t feel like you’re being difficult.
Step 9: Reconsider the drink. A large flavored lemonade, sweetened iced tea, or fruit-based cocktail can add 200 to 400 calories and 40 to 60 grams of sugar to a meal. Water with lemon, sparkling water, or unsweetened beverages are genuinely the better choice here, not as punishment, but because they let the food be the point.
Step 10: Give yourself genuine flexibility. Going out for a celebration? Having a meal you’ve been looking forward to? Eat it. Enjoy it. The goal is a sustainable pattern, not a perfect record. One genuinely indulgent meal won’t undo a week of thoughtful choices, and obsessing over every bite is its own kind of health cost.
Comparison Table: Restaurant Meals vs. Home-Cooked Equivalents
The numbers below are approximate, based on published nutritional data from major restaurant chains and standard home-cooking estimates. They illustrate the scale of difference, not exact measurements.
| Dish | Restaurant Version | Home-Cooked Version | Key Difference |
|---|---|---|---|
| Chicken stir-fry | ~1,200 cal, ~2,400 mg sodium, ~18g sugar | ~550 cal, ~700 mg sodium, ~5g sugar | Sodium 3x higher eating out |
| Caesar salad with chicken | ~800 cal, ~1,400 mg sodium, ~12g sugar | ~400 cal, ~500 mg sodium, ~4g sugar | Calories nearly double |
| Pasta with marinara | ~900 cal, ~1,600 mg sodium, ~14g sugar | ~450 cal, ~550 mg sodium, ~6g sugar | Sugar 2x from restaurant sauce |
| Grilled salmon with vegetables | ~700 cal, ~1,200 mg sodium, ~8g sugar | ~380 cal, ~400 mg sodium, ~2g sugar | Sodium 3x, even “healthy” option |
| Beef burrito | ~1,100 cal, ~2,800 mg sodium, ~6g sugar | ~550 cal, ~700 mg sodium, ~3g sugar | Sodium exceeds daily limit alone |
| Chicken noodle soup (bowl) | ~900 cal, ~2,200 mg sodium, ~6g sugar | ~350 cal, ~600 mg sodium, ~4g sugar | Sodium alone is alarming |
| Veggie burger with fries | ~1,100 cal, ~1,800 mg sodium, ~20g sugar | ~550 cal, ~600 mg sodium, ~6g sugar | Added sugars hidden in bun and sauce |
| Smoothie bowl (large) | ~780 cal, ~120 mg sodium, ~65g sugar | ~380 cal, ~60 mg sodium, ~22g sugar | Sugar almost three times as much |
Note: Home-cooked estimates assume use of minimal added salt, whole-food ingredients, and reasonable portion sizes. Restaurant values are drawn from publicly available nutritional data from major chains.
The takeaway isn’t that every restaurant meal is a disaster. It’s that the gap between what you think you’re getting and what you’re actually consuming is frequently large enough to matter over time.
Conclusion
The seed oil story is a useful case study in how dietary misinformation spreads. Take a genuine concern (ultra-processed food is making people sick), find a scapegoat that sounds scientific (seed oils), add some out-of-context data and confident-sounding influencers, and watch it go viral.
The irony is that the underlying anxiety isn’t wrong. Something genuinely is off about the modern Western diet. Chronic disease rates are rising. People feel worse, weigh more, and struggle with energy in ways that previous generations often did not. The frustration driving the seed oil discourse is legitimate. The target is just misidentified.
The truth is more complex and, in some ways, more actionable. Seed oils themselves, consumed in reasonable amounts as part of a varied diet, are not the public health crisis they’ve been painted as. The mainstream scientific consensus, from Johns Hopkins to Stanford to Memorial Sloan Kettering to the American Heart Association, is consistent on this: replacing saturated fats with polyunsaturated fats including those from seed oils is associated with better cardiovascular outcomes, not worse ones.
What IS genuinely worth your attention is the broader food environment. Ultra-processed foods, excessive sodium, hidden added sugars, distorted portion sizes, and the illusion of healthy restaurant choices are real and documented contributors to the chronic disease epidemic. These are harder villains to hate because they’re systemic and diffuse rather than bottled and labeled, but they’re the ones the evidence actually points to.
It’s worth remembering that nutrition research is genuinely complicated. Studies conflict. Individual responses to foods vary. What’s optimal for someone with cardiovascular disease may differ from what’s optimal for someone managing blood sugar. Nutritional science has gotten things wrong before, notably the decades-long demonization of dietary fat and the enthusiasm for margarine, which turned out to contain trans fats far more harmful than the butter they replaced. Humility in the face of this complexity is appropriate.
What we can say with confidence is this: a diet built around whole foods, plenty of vegetables, legumes, whole grains, lean proteins, and healthy fats, eaten mostly at home in reasonable portions, remains the most consistently health-supportive pattern in the research literature. Restaurant meals can fit into that pattern. They just require a bit more attention than most of us give them.
Eating out is a normal, pleasurable part of modern life. It doesn’t have to be an act of self-destruction, and treating it as such helps no one. But being a more informed diner, one who reads the menu a little more critically, asks a few more questions, and makes a handful of small adjustments, can genuinely shift your long-term health outcomes in meaningful ways.
The goal is not perfection. It’s awareness, applied with a light touch, over a long time.
Ready to Eat Smarter? Share This With Someone Who Eats Out Regularly.
If this article changed the way you think about restaurant food or seed oils, there’s a good chance someone in your life could use it too. Share it with a friend who’s been Googling “canola oil dangers” at midnight, or a family member who thinks their lunch salad is definitely healthy because it’s a salad.
Drop a comment below: Have you changed your oil or restaurant habits based on something you read online? We’d love to hear what you’ve tried and what actually made a difference.
Last reviewed April 2026. All nutritional claims and references are based on peer-reviewed research and guidance from major health organizations including the American Heart Association, Johns Hopkins Bloomberg School of Public Health, Stanford Prevention Research Center, and Memorial Sloan Kettering Cancer Center.