When a medication you trust turns into a weapon against your own body, it shatters more than just your health—it shatters faith in the system designed to protect you. Yet every year, pharmaceutical companies face lawsuits that reveal uncomfortable truths about how drugs reach our medicine cabinets. Most of these cases never make headlines, buried beneath corporate settlements and legal jargon that nobody reads. This is the story of eight pharmaceutical lawsuits that fundamentally altered how we think about drug safety, corporate accountability, and the price of innovation.
Table of Contents
ToggleThe Hidden Cost of Pharmaceutical Negligence
The pharmaceutical industry operates in a peculiar space where profit margins and patient safety intersect. While most medications genuinely help millions of people, the industry’s darker chapters reveal a pattern: when profits are threatened, accountability often takes a backseat. These lawsuits aren’t just legal battles—they’re windows into how corporations make decisions that affect billions of lives.
The problem runs deeper than simple greed. It’s systemic. Pharmaceutical companies invest billions in research and development, and when a drug fails to deliver expected returns, the pressure to hide problems becomes immense. Regulatory agencies, though well-intentioned, sometimes lack the resources to catch everything. This creates a perfect storm where serious side effects slip through the cracks, harming patients before anyone notices.
Understanding these cases matters because they’ve directly shaped modern drug regulation. Each lawsuit forced changes—new testing protocols, stricter labeling requirements, and increased transparency. Yet many people remain unaware of these victories because the settlements often include confidentiality clauses that silence victims.
1. Vioxx: When Pain Relief Became a Heart Attack Risk
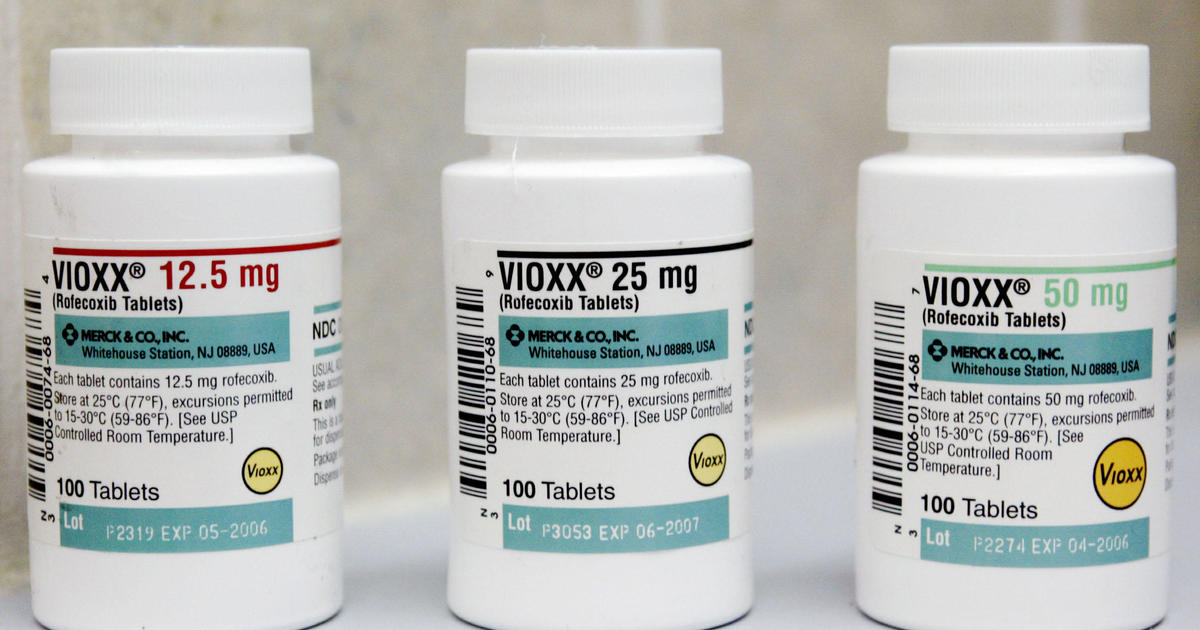
The Setup: A Drug That Seemed Too Good to Be True
In 1999, Merck introduced Vioxx (rofecoxib), a revolutionary painkiller designed specifically for arthritis sufferers. It promised relief without the stomach problems associated with traditional NSAIDs. Doctors prescribed it enthusiastically. Patients loved it. By 2004, Vioxx had generated over $2.5 billion in annual sales, making it one of the most profitable drugs ever created.
But there was a problem hiding in plain sight.
The Crisis: Internal Warnings Ignored
Merck’s own researchers discovered something alarming: Vioxx significantly increased the risk of heart attacks and strokes, particularly with long-term use. Internal emails—later revealed during litigation—showed that executives knew about these risks as early as 1996, years before the drug’s public release. Rather than halt production or issue warnings, the company allegedly downplayed the findings and continued aggressive marketing.
The consequences were staggering. An estimated 27,000 heart attacks and strokes were linked to Vioxx use. Some patients died. Others survived but faced permanent cardiac damage. The drug remained on the market for five years after Merck discovered the danger.
The Lawsuit: Justice Delayed, But Not Denied
In 2007, Merck settled a massive class-action lawsuit for $4.85 billion—the largest pharmaceutical settlement in history at that time. The company admitted no wrongdoing, a common legal maneuver that allowed executives to avoid criminal charges while still compensating victims.
Key Impact: The Vioxx case fundamentally changed how pharmaceutical companies must report safety data. It established precedent for aggressive litigation against drug manufacturers and demonstrated that even blockbuster drugs could be pulled from shelves if evidence warranted it.
2. GlaxoSmithKline’s Hidden Studies: When Data Disappears
The Deception: Selective Reporting at Its Worst
GlaxoSmithKline (GSK) manufactured Avandia, a diabetes medication that became one of the company’s cash cows. However, internal studies showed that Avandia increased the risk of heart attacks compared to competing drugs. Rather than publish these unfavorable results, GSK allegedly buried them—a practice known as “selective publication” that distorts the medical literature.
Doctors, relying on incomplete information, continued prescribing Avandia to millions of diabetic patients worldwide. The drug generated billions in revenue while patients unknowingly faced elevated cardiac risks.
The Fallout: A $3 Billion Reckoning
In 2012, GSK pleaded guilty to criminal charges and paid $3 billion in fines—the largest healthcare fraud settlement ever recorded. The company admitted to misrepresenting safety data, failing to report safety problems, and paying kickbacks to doctors who prescribed their drugs.
Critical Insight: This case exposed how pharmaceutical companies could manipulate scientific literature itself. When doctors base treatment decisions on incomplete data, patients become unwitting test subjects in a rigged experiment.
3. Merck’s Gardasil: Aggressive Marketing Meets Regulatory Pressure
The Controversy: Mandatory Vaccination Debates

Merck’s Gardasil, a vaccine preventing human papillomavirus (HPV), represented genuine medical innovation. However, the company’s aggressive marketing campaign—including lobbying for mandatory vaccination laws—raised ethical concerns about informed consent and whether the vaccine’s benefits justified the aggressive promotion.
While Gardasil itself isn’t inherently dangerous, the lawsuit centered on Merck’s marketing practices and whether the company adequately disclosed all known side effects, particularly neurological complications reported by some recipients.
The Settlement: $200 Million in Quiet Resolutions
Merck settled multiple lawsuits for approximately $200 million, though the company maintained that Gardasil’s benefits outweighed risks. The case highlighted a crucial tension: how do we balance genuine medical breakthroughs with corporate accountability for aggressive marketing?
Lesson Learned: Innovation doesn’t excuse misleading promotion. Even life-saving drugs require honest communication about risks.
4. Risperdal: Antipsychotic Drugs and Unexpected Side Effects
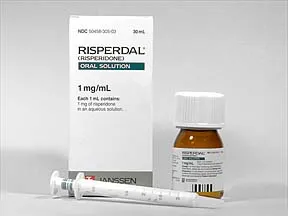
The Hidden Problem: Gynecomastia in Young Men
Johnson & Johnson’s Risperdal (risperidone) effectively treated schizophrenia and bipolar disorder, helping thousands of patients manage severe mental illness. However, the drug carried a disturbing side effect: in some young men, it caused gynecomastia—abnormal breast tissue growth—a condition that caused profound psychological distress alongside physical complications.
The company allegedly knew about this risk but failed to adequately warn prescribing physicians or patients.
The Legal Reckoning: $2.6 Billion Settlement
In 2013, Johnson & Johnson settled lawsuits for $2.6 billion, making it one of the largest pharmaceutical settlements ever. The company agreed to pay damages to thousands of men who developed gynecomastia and required surgical correction.
Why This Matters: Mental health patients are among the most vulnerable populations. When pharmaceutical companies fail to disclose side effects that could be managed with alternative treatments, they violate a sacred trust with people already struggling with serious illness.
5. Lipitor and the Diabetes Connection Nobody Wanted to Discuss

The Statins Paradox: Lowering Cholesterol, Raising Blood Sugar
Pfizer’s Lipitor (atorvastatin) became the world’s best-selling drug, prescribed to millions for cholesterol management. Clinical trials showed it reduced heart attacks and strokes. However, emerging evidence suggested that statins could increase diabetes risk, particularly in older adults—a side effect that seemed to contradict the drug’s primary benefit.
Pfizer faced allegations that it downplayed diabetes risk in marketing materials and failed to adequately warn doctors about this potential complication.
The Outcome: $650 Million Settlement
In 2012, Pfizer settled for $650 million, admitting to improper marketing practices. The company agreed to implement stricter oversight of its marketing claims and educational materials.
The Bigger Picture: This case illustrates a fundamental problem in pharmaceutical marketing: when a drug’s benefits are real but incomplete, how much responsibility do companies bear for side effects that emerge only after widespread use?
Comparative Analysis: Understanding the Pattern
| Drug | Company | Primary Issue | Settlement Amount | Year |
|---|---|---|---|---|
| Vioxx | Merck | Cardiac risks hidden | $4.85 billion | 2007 |
| Avandia | GlaxoSmithKline | Safety data buried | $3 billion | 2012 |
| Risperdal | Johnson & Johnson | Gynecomastia undisclosed | $2.6 billion | 2013 |
| Lipitor | Pfizer | Diabetes risk downplayed | $650 million | 2012 |
| Gardasil | Merck | Aggressive marketing | $200 million | 2014 |
This table reveals a disturbing pattern: major pharmaceutical companies repeatedly face massive settlements for similar violations—hiding data, downplaying risks, and aggressive marketing. Yet these companies remain profitable and continue operating largely unchanged.
6. Yaz and Yasmin: Birth Control’s Dangerous Blood Clots

The Silent Killer: Thromboembolism Risk
Bayer’s Yaz and Yasmin birth control pills promised lighter periods and clearer skin—marketing that appealed to millions of young women. What Bayer allegedly failed to adequately disclose was a significantly elevated risk of blood clots (thromboembolism) compared to older birth control formulations.
Young, healthy women—who believed they were taking a safe, routine medication—suffered strokes, pulmonary embolisms, and deep vein thrombosis. Some died.
The Litigation Explosion: $1.6 Billion Settlement
Between 2012 and 2015, Bayer settled thousands of individual lawsuits and class actions for approximately $1.6 billion. The company admitted no wrongdoing but agreed to compensate victims and their families.
Why Young Women Deserved Better: Reproductive health decisions are deeply personal. When pharmaceutical companies market birth control with incomplete safety information, they rob women of the ability to make truly informed choices about their bodies.
7. Accutane: Severe Birth Defects and Corporate Denial
The Tragedy: A Generation of Damaged Children
Roche’s Accutane (isotretinoin) effectively treated severe acne but carried a horrifying risk: if taken during pregnancy, it caused severe birth defects including cleft palate, heart abnormalities, and intellectual disability. Roche allegedly knew this risk but failed to implement adequate safeguards to prevent pregnant women from using the drug.
Thousands of children were born with preventable birth defects because their mothers, unaware of the risks, had taken Accutane during pregnancy.
The Reckoning: Multiple Settlements and Regulatory Changes
Roche faced numerous lawsuits and eventually implemented the iPLEDGE program—a strict risk management system requiring pregnancy tests and contraception verification before dispensing Accutane. While settlements totaled hundreds of millions, the real cost was measured in damaged lives.
The Lesson: Some risks are so severe that standard informed consent isn’t enough. Pharmaceutical companies must implement system-level safeguards to prevent foreseeable harms.
8. Paxil and Withdrawal: When Stopping the Drug Became Torture

The Problem: Addiction Without the Label
GlaxoSmithKline’s Paxil (paroxetine), an SSRI antidepressant, helped millions manage depression and anxiety. However, the drug created severe withdrawal symptoms when patients tried to discontinue it—symptoms so intense that many patients felt trapped, unable to stop taking the medication without experiencing debilitating side effects.
GSK allegedly downplayed withdrawal risks in marketing materials and failed to warn doctors and patients adequately about discontinuation syndrome.
The Fallout: $3 Billion in Broader Settlements
While Paxil specifically contributed to GSK’s massive 2012 settlement (mentioned earlier), the case highlighted a critical issue: pharmaceutical companies must be transparent about dependency risks, not just efficacy and common side effects.
The Human Cost: Patients felt betrayed—they’d taken medication to help their mental health, only to discover they couldn’t stop without suffering. This violated fundamental principles of autonomy and informed consent.
Why These Cases Matter More Than You Think
The Pattern of Corporate Behavior
Examining these eight cases reveals a consistent pattern: major pharmaceutical companies repeatedly prioritize profits over patient safety. They hide unfavorable data, downplay risks, and market aggressively to doctors and consumers. When caught, they pay settlements—often treated as business expenses rather than genuine accountability.
The most disturbing aspect? These companies rarely face criminal prosecution. Executives don’t go to jail. Companies pay fines but continue operating profitably. This creates a perverse incentive structure where violations become calculated business decisions rather than genuine mistakes.
The Regulatory Gap
The FDA, despite its best efforts, cannot catch everything. The agency relies partly on post-market surveillance—meaning drugs are already in patients’ bodies before comprehensive safety data emerges. Pharmaceutical companies, knowing this, sometimes take calculated risks, betting that profits will exceed eventual settlement costs.
The Human Element
Behind every lawsuit are real people: patients who trusted their doctors, who took medications believing they were safe, who suffered consequences they never anticipated. Their stories—often silenced by confidentiality agreements—deserve to be heard.
What These Lawsuits Changed (And What Still Needs Fixing)
Regulatory Improvements
These cases prompted several important changes:
- Enhanced Pharmacovigilance: Stricter requirements for reporting adverse events
- Clinical Trial Transparency: Requirements to register trials and publish results, regardless of outcomes
- Marketing Oversight: Increased scrutiny of direct-to-consumer advertising
- Label Requirements: More detailed warnings about serious side effects
What’s Still Broken
Despite these improvements, significant gaps remain:
- Settlement Confidentiality: Victims often sign agreements preventing them from discussing their cases, limiting public awareness
- Executive Accountability: Corporate fines rarely translate into personal consequences for decision-makers
- International Variation: Drugs approved in one country face different standards elsewhere, creating regulatory arbitrage opportunities
- Lobbying Power: Pharmaceutical companies spend billions lobbying regulators, creating conflicts of interest
The Role of Transparency in Modern Medicine
Why Information Matters
Every pharmaceutical lawsuit ultimately stems from information asymmetry: companies knew things about their drugs that doctors and patients didn’t. When that information gap involves safety risks, people get hurt.
Modern medicine requires radical transparency. Patients deserve to know:
- All clinical trial results, including negative findings
- Known side effects, even rare ones
- How the drug compares to alternatives
- What the company knew and when they knew it
The Internet’s Double-Edged Sword
Social media and online communities have made it harder for pharmaceutical companies to suppress information. Patients connect, share experiences, and collectively piece together patterns that individual doctors might miss. While this creates challenges for companies, it ultimately serves patients better.
Moving Forward: What Patients Should Know
Questions to Ask Your Doctor
When prescribed a new medication, ask:
- What are all known side effects, including rare ones?
- How does this drug compare to alternatives?
- What clinical evidence supports this choice for my specific situation?
- Are there any recent lawsuits or safety concerns?
- How will we monitor for adverse effects?
Resources for Research
- ClinicalTrials.gov: Access to clinical trial data
- FDA Adverse Event Reporting System (FAERS): Real-world safety data
- PubMed: Medical literature database
- DrugWatch.com: Lawsuit and safety information
The Power of Informed Consent
Informed consent isn’t just a legal requirement—it’s a fundamental right. You deserve complete, honest information about medications affecting your health. If your doctor seems dismissive of questions or unwilling to discuss risks, that’s a red flag.
Conclusion: The Ongoing Battle for Accountability
These eight pharmaceutical lawsuits represent victories for patients and transparency, yet they also reveal how much work remains. Every settlement, every regulatory change, every exposed cover-up represents lives that could have been protected earlier.
The pharmaceutical industry has genuinely improved medicine. Vaccines save millions. Antibiotics conquered infections that once meant death. Cancer drugs offer hope where none existed. But innovation doesn’t excuse negligence, and profit doesn’t justify deception.
As patients, we must remain vigilant. We must ask questions, demand transparency, and hold companies accountable. We must support regulatory agencies with adequate funding and independence. We must ensure that the next generation of medications reaches patients through honest channels, with complete information about both benefits and risks.
The lawsuits discussed here aren’t just legal cases—they’re reminders that behind every medication is a company making choices. Those choices should prioritize human health above quarterly earnings. Until they consistently do, cases like these will continue to emerge, and patients will continue to suffer preventable harm.
The question isn’t whether pharmaceutical companies will face more lawsuits. It’s whether we’ll demand the systemic changes necessary to prevent the next scandal before it harms millions.